In this article:
- What is Bronchitis?
- Causes of Bronchitis
- Key Symptoms of Bronchitis
- Diagnosis of Bronchitis
- Complications of Chronic Bronchitis
- Treating Bronchitis Symptoms
- Preventive Measures
- When to Seek Medical Attention
What Is Bronchitis?
Definition and Overview
Bronchitis is a respiratory infection, often described as a chest cold, that causes inflammation in the bronchial tubes, also called the bronchi. These airways carry air from the trachea down into the lungs and are essential for normal breathing. When the lining of these airways becomes irritated or infected, the respiratory tract produces more mucus than usual.
As the mucus builds up, the airways become swollen and congested, which leads to persistent coughing and chest discomfort. In primary care settings across Georgia, this type of respiratory condition is a common reason patients seek care for persistent cough and chest tightness.
Types: Acute vs. Chronic
Doctors generally describe bronchitis as either acute bronchitis or chronic bronchitis, two common types of respiratory tract infections affecting the airways.
Acute bronchitis is the type most people experience, especially following respiratory viruses. It often begins after a cold or flu that gradually moves into the chest. Chronic bronchitis, however, is a long-term respiratory condition linked to chronic obstructive pulmonary disease, or COPD.
Instead of resolving within a few weeks, chronic bronchitis involves ongoing airway inflammation and a productive cough that can persist for months and sometimes longer.
Causes of Bronchitis
Viral Infections
For most adults who develop bronchitis, the cause is a viral infection. In fact, the same viruses that cause common respiratory illnesses can also inflame the airways in the chest. Respiratory viruses such as influenza, COVID-19, rhinovirus, adenovirus, and Respiratory syncytial virus are frequent triggers. Quite often, the illness begins with what feels like a typical cold. You may notice a sore throat, mild congestion, or fatigue at first. However, as the respiratory infection progresses, the inflammation can affect the bronchial airways.
Because viruses irritate the airway lining, the respiratory tract produces more mucus, which leads to the persistent cough many people associate with bronchitis.
Smoking and Irritants
While viral infections are the most common cause, irritation in the airways can also trigger bronchitis. In less common cases, bacteria such as bordetella pertussis, chlamydia pneumoniae, or mycoplasma pneumoniae may also contribute. Substances such as cigarette smoke, secondhand smoke, air pollution, and certain chemical irritants can inflame the lining of the respiratory tract.
Over time, repeated exposure can weaken normal lung function and make the airways more sensitive to infection. As a result, people who regularly breathe in these irritants may experience bronchitis more often. In some individuals, long-term irritation can even contribute to chronic bronchitis, a condition linked to chronic obstructive pulmonary disease.
Key Symptoms of Bronchitis
Bronchitis symptoms often begin after a cold and gradually shift into the chest, with a deeper cough, heaviness, and tighter breathing. Because the airways are affected, symptoms tend to center in the chest and follow a recognizable pattern that may worsen over time, leading many patients to seek evaluation.
At AllCare, our primary care team offers convenient visits across Georgia to assess symptoms and help determine the next steps for treatment.
Persistent Cough
The most recognizable symptom of bronchitis is a persistent cough that often starts like a cold and becomes deeper and more noticeable. As the airways become inflamed, excess mucus builds in the chest, triggering coughing to help clear it.
Common cough symptoms with bronchitis include:
- A cough that brings up mucus or sputum. This mucus may appear clear, yellow, or slightly green as the infection develops.
- Frequent sputum production. The respiratory tract produces extra mucus as the airways become irritated.
- Coughing fits triggered by deep breaths. Even a single deep breath, laughing, or talking can suddenly trigger a coughing spell.
- A cough that lingers throughout the day and often worsens at night.
Chest Discomfort
Chest discomfort is common with bronchitis and may feel like tightness, soreness, or mild pain. It is often caused by repeated coughing and airway inflammation, which can create a sense of pressure or heaviness in the chest.
Wheezing
Wheezing occurs when air moves through narrowed, inflamed airways, producing a soft whistling sound. It may be accompanied by mild shortness of breath, making activities like walking or climbing stairs feel more tiring.
Nasal Congestion
Bronchitis often starts like a cold with nasal congestion, a runny nose, or sore throat before moving into the chest, where a heavier cough and increased mucus develop.
Diagnosis of Bronchitis
Clinical Evaluation
If you have been coughing for several days and the symptoms are not improving, it is natural to want clear answers about what is going on. When a healthcare provider at AllCare evaluates possible bronchitis, the process usually begins with a clinical exam rather than a long list of tests.
The doctors in our offices will talk through your symptoms, including a persistent cough, mucus production, chest congestion, fatigue, and any changes in breathing.
During the visit, they will listen to your lungs with a stethoscope, checking for signs such as wheezing, airway congestion, or reduced airflow. At AllCare, providers across Georgia evaluate these symptoms daily, helping patients distinguish between bronchitis and other respiratory conditions.
At the same time, the doctor considers other possible causes of cough, including seasonal allergies, which are very common in high-pollen regions of the Southeast. Allergies often cause sneezing, itchy eyes, and a dry cough without fever. Bronchitis, on the other hand, usually brings a deeper chest cough with mucus that gradually worsens over several days and may include a low-grade fever.
Differentiating from Pneumonia
After several days of coughing, many people begin to worry that the illness may have progressed beyond bronchitis to pneumonia. The symptoms can feel similar at first, which is why clinicians look carefully for certain warning signs. These include higher or persistent fever, noticeable shortness of breath, rapid or labored breathing, and chest discomfort or chest pain when taking deep breaths.
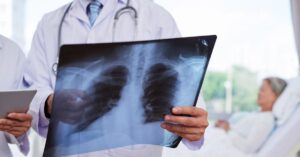
During the exam, providers listen closely to the lungs for abnormal sounds or areas where airflow seems reduced. If those findings raise concern, a chest X-ray may be recommended to check for infection in the lungs. An in-person evaluation can help determine whether the illness is bronchitis or pneumonia.
Laboratory Tests
Bronchitis usually does not require extensive testing for diagnosis. Providers often recognize the condition based on symptoms and a lung exam. However, when symptoms last longer than expected or do not follow the usual pattern, additional tests such as blood tests, sputum testing, pulmonary function tests, or spirometry may be used to assess lung function.
Complications of Chronic Bronchitis
Long-term Health Risks
Chronic bronchitis differs from acute bronchitis because it is not a temporary infection and involves ongoing airway inflammation. It is a form of COPD (chronic obstructive pulmonary disease), which gradually damages the airways, limits airflow, and reduces lung function.
As inflammation and mucus build, symptoms may include a persistent cough, repeated respiratory infections, and reduced lung capacity.
Early management can help protect lung health, and pulmonary rehabilitation may be recommended to improve breathing.
Impact on Quality of Life
Living with chronic bronchitis can gradually make everyday breathing feel like a challenge. Some of the ongoing symptoms include coughing, persistent mucus, and shortness of breath.
Over time, these symptoms can lower energy levels and make simple tasks feel more tiring. Activities such as walking, climbing stairs, or exercising may begin to take more effort as breathing and overall lung function slowly become more limited.
Continued structured support such as regular primary care and pulmonary rehabilitation can help improve endurance over time.
Treating Bronchitis Symptoms
Over-the-Counter Medications
Treatment for bronchitis focuses on relieving symptoms while the body clears the infection. Over-the-counter medications such as cough suppressants, guaifenesin (which helps thin mucus), and dextromethorphan (which helps reduce coughing) may provide relief. However, these medications do not treat the underlying infection. Because coughing helps clear mucus from the airways, it should not be suppressed too aggressively.
Home Remedies and Lifestyle Changes
Simple home remedies can help relieve bronchitis symptoms as the body recovers. Using a humidifier, staying hydrated, and getting rest can loosen mucus and ease coughing, while honey may help soothe symptoms at night. Most symptoms improve within 7–10 days, though the cough can last several weeks.
When to Avoid Antibiotics
Many people wonder whether antibiotics will help bronchitis symptoms improve faster. In reality, most cases of acute bronchitis are caused by viral infections, which means antibiotics are not effective. This form of illness is often referred to as acute viral bronchitis.
In some situations, a doctor may consider the possibility of bacterial bronchitis. This may be more likely if symptoms worsen instead of improving, if a higher or persistent fever develops, or if the illness lasts longer than expected.
Because these situations can look similar to other respiratory infections, determining whether antibiotics are appropriate usually requires an in-person medical evaluation with a healthcare provider, such as AllCare.
Preventive Measures
Vaccination
Vaccines can play an important role in protecting the lungs from respiratory infections that sometimes lead to bronchitis. Staying current with recommended vaccines helps strengthen the body’s defense during peak virus seasons. The influenza vaccine and the COVID-19 vaccine both help lower the risk of serious respiratory illness. Even if infection occurs, vaccines often make symptoms milder and allow the respiratory system to recover more smoothly.
Lifestyle Modifications
Small everyday habits can also help protect the airways and support long-term respiratory health. Avoiding smoking and secondhand smoke is one of the most effective ways to reduce irritation in the lungs. Limiting exposure to air pollution when possible may also help protect the respiratory tract. In addition, getting enough sleep, staying hydrated, and practicing good hygiene support the immune system and may reduce the risk of repeated bronchitis episodes.
When to Seek Medical Attention
Persistent or Worsening Symptoms
Most bronchitis cases improve over time, but medical care may be needed if symptoms worsen. Seek evaluation for fever above 100.4°F, increasing shortness of breath, strained breathing, discolored or bloody mucus, symptoms lasting more than 10 days, or a cough that persists beyond three weeks.
Preventing Complications
Getting medical guidance early can help confirm the diagnosis and rule out more serious conditions such as pneumonia. Many people wait, hoping the symptoms will pass. If you are unsure whether your illness is bronchitis or something else, a visit to a medical professional can provide clarity and a clear path toward feeling better.
At AllCare, our team offers convenient primary and immediate care visits across Georgia to evaluate ongoing respiratory symptoms.