In this article:
- Understanding Pneumonia: An Overview
- What is Pneumonia?
- Causes of Pneumonia
- Key Symptoms of Pneumonia
- How Symptoms Vary Across Age Groups
- Types of Pneumonia Based on Acquisition
- Understanding Early Warning Signs
- Risk Factors and Vulnerable Groups
- Diagnosing Pneumonia
- Treatment Options
- Potential Complications of Pneumonia
- Preventative Measures
- Conclusion: Managing and Mitigating Pneumonia
Understanding Pneumonia: An Overview
Pneumonia is a lung infection that affects breathing and daily function. It occurs when the tiny air sacs in the lungs, called alveoli, become inflamed and fill with fluid or pus, making it harder for oxygen to reach the bloodstream. As a result, even simple activities can feel exhausting. In primary care settings across Georgia, pneumonia is a common reason patients seek care for ongoing cough, fever, or breathing changes.
Pneumonia can be bacterial, viral, or fungal. In adults, bacterial pneumonia is most common, though viral infections can cause similar symptoms. Some cases are mild, often called walking pneumonia, while others are more serious and require medical care, meaning pneumonia exists on a spectrum.
In Georgia, where long allergy seasons and humidity are common, early symptoms can resemble a cold or respiratory irritation, making it harder to recognize when something more serious is developing.
What is Pneumonia?
To understand pneumonia, it helps to picture what’s happening in the lungs. In healthy lungs, tiny air sacs called alveoli stay open and filled with air, allowing oxygen to pass into the bloodstream. With pneumonia, these air sacs become inflamed as the body responds to infection. White blood cells move in, and fluid or pus builds up where air should be.
This buildup limits oxygen exchange, leading to symptoms like coughing, chest discomfort, and difficulty taking a full breath. Breathing can feel heavier and more tiring than with a typical respiratory illness or lung infection.
That’s what sets pneumonia apart from a cold or flu. While those affect the upper respiratory system, pneumonia reaches deeper into the lungs, where symptoms become more intense and harder to ignore.
Causes of Pneumonia
Pneumonia often starts as a respiratory infection, like a cold or flu, with mild symptoms that worsen instead of improving.
Here’s how that progression happens:
- A viral infection weakens the airway lining
- Bacteria, viruses, or other germs move into the lungs
- The infection causes inflammation and fluid buildup
With a cold, symptoms improve over time. With pneumonia, symptoms may worsen, leading to a deeper cough, fever, or trouble breathing.
Bacterial Pneumonia
Bacterial pneumonia is the most common type in adults and is often caused by bacteria like pneumococcal pneumonia or Mycoplasma pneumoniae, a common cause of walking pneumonia.
A common pattern:
- You start recovering from a cold or flu
- Then symptoms suddenly get worse
- A cough becomes more persistent and produces mucus
Because this is a bacterial infection, antibiotics are usually needed. Without treatment, symptoms can continue to worsen.
Viral Pneumonia
Viral pneumonia is caused by viruses like the flu, RSV, or COVID-19. Some milder cases may resemble walking pneumonia, though symptoms can still worsen over time.
You may notice:
- Ongoing cough and fatigue
- Fever and body aches
- Gradually increasing shortness of breath
Antibiotics do not treat viral pneumonia. Care focuses on rest and supportive treatment while the immune system fights the infection, though symptoms may still worsen.
Fungal Pneumonia
Fungal pneumonia is less common and usually affects people with weakened immune systems.
- Caused by fungal spores entering the lungs
- More likely in people with underlying conditions
- Symptoms may develop more gradually
Although rare, it still requires medical evaluation and treatment. Some atypical infections, including those caused by mycoplasma pneumonia, may develop more gradually.
Key Symptoms of Pneumonia
Pneumonia symptoms can start off feeling similar to a cold or the flu. However, instead of improving over time, they often become more intense, last longer, and feel deeper in the chest. You may notice a combination of symptoms, including:
- A persistent cough that doesn’t go away
- Fever with chills or sweating
- Shortness of breath, even with light activity
- Chest pain when breathing or coughing
- Ongoing fatigue or weakness
Pneumonia symptoms often worsen or linger instead of improving. If symptoms continue to progress, a provider like AllCare can help determine if pneumonia is developing.
Persistent Cough
A cough is one of the most common symptoms of pneumonia, but it often feels different from a typical cold. You may notice:
- A persistent cough that doesn’t improve
- Coughing that feels deeper in the chest
- Thick or discolored mucus (yellow, green, or rust-colored)
This type of cough is your body’s way of trying to clear fluid from the lungs, which is why it can feel more intense and harder to control.
Fever and Chills
Fever is a common sign that your body is fighting an infection, but with pneumonia, it can feel more pronounced and last longer. You may notice:
- A higher or lingering fever
- Chills that come and go
- Sweating, especially at night
Difficulty Breathing
As pneumonia affects the lungs, breathing can start to feel more difficult. You may notice:
- Shortness of breath during normal activities
- A feeling that you can’t take a full, deep breath
- Faster or more shallow breathing
Chest Pain
Chest pain with pneumonia is often linked to inflammation in the lungs and surrounding tissues. You may notice:
- Sharp or stabbing chest pain
- Pain that worsens with deep breathing or coughing
- Discomfort that feels centered in the chest
This type of pain can be a key sign that the infection has moved beyond the upper respiratory system.
Fatigue and Weakness
Fatigue with pneumonia often feels more intense than typical tiredness from a cold. You may notice:
- Ongoing exhaustion, even after rest
- Low energy throughout the day
- A general sense of weakness
This is one of the most noticeable symptoms. Research shows fatigue and weakness are among the most common in pneumonia and can significantly impact daily activities.
How Symptoms Vary Across Age Groups
Pneumonia doesn’t look the same for everyone. While many adults have symptoms like cough, fever, and shortness of breath, children and older adults may show more subtle signs. Because of this, it’s important to watch for changes in behavior, energy, or breathing, especially in higher-risk groups.
Pediatric Symptoms
In children, pneumonia symptoms can develop quickly and may look different from what adults experience. While fever and cough are still common, some signs can be more subtle or easy to overlook. You may notice:
- Rapid or labored breathing
- Fever that doesn’t improve
- Flaring nostrils or visible effort when breathing
- Decreased appetite or low energy
In younger children, symptoms may not always be clearly expressed, so changes in breathing or behavior are often the first indicators that something more serious is going on.
Symptoms in the Elderly
In older adults, pneumonia symptoms may not follow the typical pattern. Instead of a strong cough or high fever, the first signs can be more subtle and sometimes unexpected. You may notice:
- Confusion or changes in mental clarity
- Increased fatigue or weakness
- Reduced appetite
- Mild or absent fever
This type of presentation is important to recognize, as confusion or altered mental status can sometimes be one of the earliest signs of pneumonia in older adults.
Types of Pneumonia Based on Acquisition
Pneumonia can start in different ways depending on where the infection begins. For example, it may develop after a cold at home, during a hospital stay, or from food or liquid going down the wrong way. These differences help explain why symptoms and treatment can vary.
Community-Acquired Pneumonia
Community-acquired pneumonia is the most common type and develops outside of a hospital, often after a cold, flu, or another respiratory illness. Symptoms typically worsen instead of improving, with a deeper cough, lower energy, and more difficult breathing.
Hospital-Acquired Pneumonia
Hospital-acquired pneumonia, also called healthcare-acquired or nosocomial pneumonia, develops during or after a hospital stay. It often affects people already dealing with other health issues and may involve harder-to-treat bacteria, leading to faster or more severe symptoms.
Aspiration Pneumonia
Aspiration pneumonia occurs when food, liquid, saliva, or small particles enter the lungs instead of the stomach. This is more common in people with swallowing difficulties or certain medical conditions. Sometimes it’s subtle, such as microaspiration, where small amounts enter the lungs unnoticed and can lead to infection over time. Because of this, symptoms may be harder to connect to a specific moment.
Understanding Early Warning Signs
Some pneumonia symptoms can be monitored at home, but others signal the infection may be worsening and need medical attention. Paying attention to symptom progression is key.
Watch for these red flag symptoms:
- Difficulty breathing or noticeable shortness of breath, especially at rest
- A fever above 102°F that does not improve with medication
- Bluish lips or fingernails, which can signal low oxygen levels
- Chest pain that worsens with breathing or coughing
- Confusion, trouble focusing, or unusual behavior
- Symptoms that suddenly worsen after seeming to improve
These signs can vary by age. Children may show rapid breathing or increased effort, while older adults may experience confusion or sudden fatigue. If you notice any of these changes, it’s a good idea to contact a healthcare provider or seek care right away.
Risk Factors and Vulnerable Groups
While pneumonia can affect anyone, certain risk factors make it more likely to develop or become more serious. Some people are more at risk for pneumonia than others. In many cases, it comes down to how well the immune system can respond to an infection. When the immune system is weakened or already under strain, the body has a harder time fighting off bacteria or viruses that reach the lungs.
Some of the most common risk factors include:
- Age, especially in very young children and older adults
- Chronic conditions like asthma, COPD, or diabetes
- A weakened immune system due to illness, medications, or ongoing treatment
- Recent respiratory infections that have not fully resolved
For parents, one common question is whether mild or “outgrown” asthma still matters. In many cases, it can. Even if symptoms are no longer obvious, a history of asthma can still make the airways more sensitive and increase the risk of complications with respiratory infections. Understanding these risk factors can help you take symptoms seriously earlier and decide when it’s time to seek care.
Diagnosing Pneumonia
If pneumonia is suspected, a healthcare provider will focus on a few key things to make a diagnosis. The goal is to understand your symptoms and confirm whether the infection has reached the lungs. Most visits are straightforward and move quickly.
At your appointment, you can expect:
- Questions about your symptoms and how they’ve changed over time
- A review of your recent illness or medical history
- A physical exam to check your breathing
In some cases, that’s enough to make a diagnosis. If not, additional medical testing may be used to confirm it.
Medical History and Physical Exam
The first step is a conversation. A doctor will ask about your symptoms, including coughing, fever, and shortness of breath, and whether they are improving or getting worse. In some cases, blood tests may also be used to better understand the severity of the infection.
Then, they will listen to your lungs using a stethoscope. Certain sounds, like crackling or reduced airflow, can be early signs of pneumonia. This quick exam often gives strong clues about what’s going on.
Diagnostic Tests and Imaging
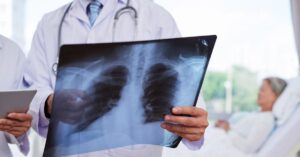
If the diagnosis is not clear, imaging or tests may be needed. The most common is a chest X-ray, which can show fluid or inflammation in the lungs.
You may also have:
- Blood tests to check for infection
- Other diagnostic tests if symptoms are more severe
These tools, including a chest x-ray, help confirm pneumonia and guide the right treatment.
Treatment Options
Treatment for pneumonia depends on what’s causing the infection and how severe the symptoms are. Some cases can be managed at home, while others may need closer medical care. The goal of treatment is to clear the infection, support breathing, and help your body recover. The physicians at AllCare can help determine which approach is appropriate based on your symptoms.
Most treatment plans include:
- Targeting the cause of the infection (bacterial vs viral)
- Managing symptoms like fever, cough, and discomfort
- Supporting the body with rest and hydration
Antibiotic Treatment for Bacterial Pneumonia
Bacterial pneumonia is treated with antibiotics, which are needed to clear the infection from the lungs. Once treatment starts, many people begin to feel some improvement within a few days.
With antibiotics, you can expect:
- Gradual reduction in fever and symptoms
- Less mucus and coughing over time
- Improved energy as the infection clears
It’s important to take the full course of antibiotics, even if you start to feel better. Stopping early can allow the infection to return or worsen.
Supportive Care for Viral Pneumonia
Viral pneumonia does not respond to antibiotics, so treatment focuses on helping your body recover. In many cases, your immune system will clear the infection with time and supportive care.
Treatment typically includes:
- Rest to allow the body to heal
- Fluids to stay hydrated and loosen mucus
- Over-the-counter medications for fever and discomfort
Recovery may take a little longer, and symptoms can linger. It’s normal to feel tired even after other symptoms begin to improve.
Potential Complications of Pneumonia
Most cases of pneumonia improve with the right treatment, but if it’s left untreated or becomes more severe, complications can develop. This is why it’s important to pay attention to symptoms and seek care when they worsen instead of waiting it out.
Some possible complications include:
- Fluid buildup around the lungs, called pleural effusion, which can make breathing more difficult
- Worsening infection that spreads deeper into the lungs
- Low oxygen levels that may require additional support
- Hospitalization for more advanced care and monitoring
These complications are more likely in people with underlying health conditions or a weakened immune system. The good news is that early diagnosis and treatment can help prevent most of these issues and lead to a smoother recovery.
Preventative Measures
While pneumonia isn’t always preventable, simple steps can lower your risk by protecting your lungs and supporting your immune system. In Georgia, where long allergy seasons and humidity can make symptoms linger, it can be harder to tell irritation from infection. That’s why it’s important to stay proactive and check in with a primary care provider if symptoms persist or feel unusual.
A few ways to reduce your risk include:
- Staying up to date on recommended vaccines
- Treating colds and respiratory symptoms early
- Practicing good hygiene, especially during cold and flu season
- Supporting your immune system with rest and hydration
Vaccination
Vaccines are one of the most effective ways to help prevent certain types of pneumonia and related infections. They work by preparing your immune system to recognize and respond to specific bacteria or viruses.
Common vaccines include:
- Pneumococcal vaccines, which protect against a common cause of bacterial pneumonia
- Flu vaccine, which helps reduce the risk of complications that can lead to pneumonia
- COVID-19 vaccine, which can prevent severe respiratory illness
- RSV vaccine, recommended for certain age groups and higher-risk individuals
Staying up to date with these vaccines can significantly reduce your risk of serious illness.
Hygiene and Lifestyle Adjustments
Everyday habits also play a big role in prevention. Small actions can help limit exposure to germs and support overall lung health.
Helpful habits include:
- Washing your hands regularly
- Avoiding close contact with people who are sick
- Covering your mouth when coughing or sneezing
- Getting enough rest and staying hydrated
These steps may seem simple, but they can make a meaningful difference, especially during times of year when respiratory illnesses are more common.
Conclusion: Managing and Mitigating Pneumonia
Pneumonia may start like a routine illness, but symptoms often worsen over time. A deeper cough, ongoing fever, shortness of breath, or chest pain may signal something more serious. With early diagnosis and treatment, most cases improve without complications.
If your symptoms are not getting better or are starting to worsen, it’s time to take the next step. Getting evaluated sooner can make a real difference in how quickly you recover.
At AllCare, our team can assess your symptoms, provide a clear diagnosis, and start the right treatment plan right away.
You can:
- Book an appointment with AllCare
- Visit one of our urgent care locations for a same-day evaluation
- Contact your primary care physician if that’s your usual route
Taking action early can help you get the care you need and start feeling better sooner.